Monday, April 03, 2017 9:06:21 AM
Added PR Notes to AACR’17/#1651 PPHM+MSK “Bavi+ACT/CAR T”
4-3-17/8am #1651 - Session: TUMOR MICROENVIRONMENT & CHECKPOINTS [Joint PPHM & Memorial Sloan Kettering]
“Targeting Phosphatidylserine in Combination with Adoptive T Cell Transfer Eliminates Advanced Tumors without Off-Target Toxicities in a Melanoma Preclinical Model” <=NEW(2nd) MSK STUDY
=> Daniel Hirschhorn-Cymerman 1, Sara Sara Schad 1, Sadna Budhu 1, Zhong Hong 1, Xia Yang 1, Hutchins T. Jeff 2, Bruce D. Freimark 2, Michael J. Gray 2, Jedd Wolchok 1, Taha Merghoub [Memorial Sloan Kettering]
1=Memorial Sloan Kettering CC, NYC [ http://www.mskcc.org/research-areas/labs/jedd-wolchok ]
2=Peregrine Pharmaceuticals
ABSTRACT:
A viable strategy to treat advanced cancers includes transferring of tumor-specific T cells. T cells that recognize tumor antigens can be expanded and reinvigorated ex-vivo. Furthermore, autologous T cells can be genetically modified to express anti-tumor T cell receptors [TCRs] or chimeric antigen receptors [CARs]. Although the potency and specificity of tumor-specific T cells can be manipulated ex-vivo, once re-infused into patients, the T cells are subjected to immunosuppressive mechanisms established by the tumor. An important immune checkpoint regulator within tumors is phosphatidylserine (PS). Innate immune cells exposed to PS secrete suppressive cytokines and chemokines that can significantly impair the function and activation of anti-tumor T cells. Therefore, monoclonal antibodies that block PS activity can increase the anti-tumor potency of transferred T cells to treat aggressive cancers. Here we show that a PS targeting monoclonal antibody in combination with CD4+ T cells that recognize the melanoma antigen Trp1 can regress very advanced melanomas in all treated mice. Combination of anti-Trp1 CD4+ T cells with other immunomodulatory modalities such as anti-OX40 antibodies, can achieve equivalent treatment rates but these are typically accompanied by severe immune related adverse events. In contrast, in this setting, PS blockade did not show any off-target toxicities. Flow cytometry analysis revealed lower levels of CD206 expression concomitant with higher activation markers in macrophages and neutrophils in tumors from anti-PS treated mice. These results suggest that diminishing suppressive mechanisms locally in adoptive transfer protocols is a highly desirable strategy that can eliminate tumors while minimizing related adverse events.
---------------------
FROM PPHM’s 4-3-17 PR: http://ir.peregrineinc.com/releasedetail.cfm?ReleaseID=1019762
…”Latest Findings from Ongoing Collaboration with Memorial Sloan Kettering (MSK) Support Potential Applications for Combining CAR T & Anti-PS in Treatment of Solid Tumors”… For this study, a team of MSK researchers led by cancer immunotherapy thought-leaders, Taha Merghoub, Ph.D. and Jedd D. Wolchok, M.D., Ph.D., evaluated and compared the anti-tumor activity and off-target toxicities of adoptive T cell transfer therapy in combination with either PS-targeting antibodies or anti-OX40 antibodies in mice with advanced melanomas. Whereas PS-targeting and anti-OX40 demonstrated comparable tumor regression when administered in combination with transferred adoptive T cells, only the PS-targeting combination achieved these results without any off-target toxicities. By contrast, the anti-OX40 treatment combination triggered off-target inflammatory destruction of healthy tissues. Additional study results demonstrated that the PS-targeting antibodies decreased tumor-induced immunosuppression as evidenced by a decrease in immunosuppressive regulatory T cells (Tregs) and M2 macrophages. This finding is consistent with Peregrine’s belief that bavituximab may modulate the immunosuppressive tumor microenvironment and enhance the activity of immunotherapy agents.
Taha Merghoub, Ph.D., Co-Dir. of the Ludwig Collaborative Laboratory at MSK:
“While adoptive T cell transfer remains one of the most exciting new approaches to treating cancer, to date the toxicity associated with the treatment has limited its potential. We are encouraged that these study results showed that the combination of anti-PS and adoptive T cell treatment led to enhanced anti-tumor effect without any evidence of additional off-target side effects. “We believe that these findings may support potential applications for this combination in solid tumors in the future.”
Joseph Shan, Peregrine’s VP of Clinical & Regulatory Affairs:
“These study results provide further support for our belief that anti-PS agents such as bavituximab can play an important role as part of combination cancer treatments. This is directly tied to the agents’ ability to modulate the tumor microenvironment to combat the immunosuppression that limits the activity of CAR T and immunotherapies. Importantly, we are now also seeing evidence that this targeted modulation of the tumor microenvironment by anti-PS allows for enhanced activity of these other treatments without triggering any off-target toxicities. This is opposed to other conventional immunotherapies such as anti-OX40 with systemic mechanisms of action. We believe this advantageous tolerability profile will be a key benefit in positioning anti-PS agents for inclusion in optimal combination cancer regimens.”
---------------------
8-2015: Presently there are 3 types of Adoptive Cell Transfer (ACT) using effector T cells that are advancing on a path towards regulatory approval:
1. TILs (tumor infiltrating lymphocytes) have been developed with slow but continuing progress over several decades.
2. CARs (chimeric antibody receptors) – newer gene-modified T cells strategy
3. TCRs (T-cell receptors) – newer gene-modified T cells strategy
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4507286/
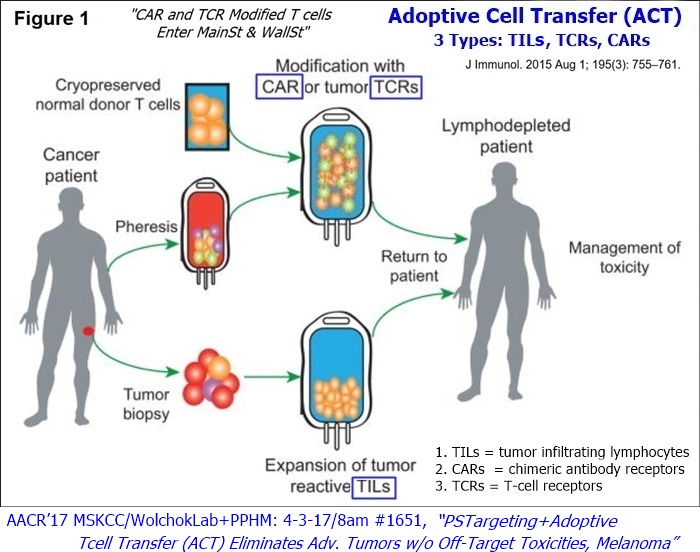
...“Adoptive T cell transfer is like ‘giving patients a living drug’,” states Renier J. Brentjens, MD/PhD, of Memorial Sloan Kettering Cancer Center (MSKCC).
… https://www.cancer.gov/about-cancer/treatment/research/car-t-cells
...“Adoptive T cell therapy (ACT) is one stone in this new pillar, a potentially powerful approach to cancer treatment that relies on the infusion of tumor-specific T cells.”
… https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4327320
= = = = = = = = =
Interesting 3-31-17 Sloan Kettering Tweet re: AACR’17
3-31-17 9:20amET “Getting ready for #AACR17? #Immunotherapy will be a hot topic. Learn more about how it works (video). @AACR”
https://twitter.com/sloan_kettering
Points to this 4-2016 Video (1:20):
“Immunotherapy – How It Works” https://www.youtube.com/watch?v=COQ1AeoGyco
Beg@:39:
“Immunotherapy drugs release this brake and empower immune cells to fight the cancer.
Sometimes the immune system needs a tune-up before it can fight cancer.
Immune cells can be removed from the body, armed with new proteins that can target cancer cells, and given back to a patient in large numbers.
Once inside the body, the modified immune cells recognize and attack the cancer.
This approach is called CAR T cell therapy. [an Adoptive Cell Transfer “ACT” strategy]
Despite the promise of immunotherapy, not everybody responds.
MSKCC scientists are exploring ways to improve immunotherapy.”

=============AND, THIS 3-23-17 PARKER FOUNDATION RELEASE ON AACR’17:
3-23-17: “Parker Institute for Cancer Immunotherapy Scientists to Present Research on Checkpoint Inhibitors, Adoptive Cell Therapy, and Other Advances in Immuno-oncology at AACR 2017”
Investigators affiliated with the Parker Institute for Cancer Immunotherapy will present some of the most anticipated immuno-oncology research at the 2017 AACR Annual Meeting. The event takes place at the Walter E. Washington Convention Center in Washington, DC, April 1-5 2017. . .
Other adoptive cell therapy abstracts of interest:
• ”Targeting Phosphatidylserine in Combination with Adoptive T Cell Transfer Eliminates Advanced Tumors without Off-Target Toxicities in a Melanoma Preclinical Model” [see http://tinyurl.com/nx5q5os ]
The principal investigator is Taha Merghoub, PhD, Parker Institute member researcher at Memorial Sloan Kettering Cancer Center. Co-authors include Parker Institute Center Director Jedd Wolchok, MD, PhD, at Memorial Sloan Kettering Cancer Center.
http://www.parkerici.org/media/2017/parker-institute-for-cancer-immunotherapy-scientists-to-present-research-on
----------ACT NOTES:
NOTE1:
From 3-2014 Immunotherapy article: “Cancer immunotherapy, particularly adoptive cell transfer (ACT), has shown great promise in the treatment of patients with late-stage disease, including those who are refractory to std. Therapies” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4372895
NOTE2:
The Parker Foundation: “The Immunotherapy Dream Team”
Through the support from SEAN PARKER, Stand Up To Cancer (SU2C) and the Cancer Research Institute (CRI) formed an Immunology Research Dream Team dedicated to cancer immunology: “Immunologic Checkpoint Blockade & Adoptive Cell Transfer in Cancer Therapy.” The Immunotherapy Dream Team is focused on 2 approaches for this translational cancer research project, which will unite laboratory & clinical efforts towards the immunological treatment, control, and prevention of cancer.
The 1st is investigating blockades (by inhibitory molecules called “checkpoints”) of T lymphocytes’ inhibitory receptors, which block immune responses; and the use of antibodies to remove the checkpoints, once again allowing white blood cells called T lymphocytes to kill the cancer cells.
Second, the Immunotherapy Dream Team is pursuing multiple Adoptive Cell Transfer (ACT) approaches, which increase immunity.”
DREAM TEAM LEADERSHIP: 10 scientists, incl. MSKCC’s Jedd D. Wolchok & Michel Sadelain.
http://parker.org/initiatives/immunotherapy
4-3-17/8am #1651 - Session: TUMOR MICROENVIRONMENT & CHECKPOINTS [Joint PPHM & Memorial Sloan Kettering]
“Targeting Phosphatidylserine in Combination with Adoptive T Cell Transfer Eliminates Advanced Tumors without Off-Target Toxicities in a Melanoma Preclinical Model” <=NEW(2nd) MSK STUDY
=> Daniel Hirschhorn-Cymerman 1, Sara Sara Schad 1, Sadna Budhu 1, Zhong Hong 1, Xia Yang 1, Hutchins T. Jeff 2, Bruce D. Freimark 2, Michael J. Gray 2, Jedd Wolchok 1, Taha Merghoub [Memorial Sloan Kettering]
1=Memorial Sloan Kettering CC, NYC [ http://www.mskcc.org/research-areas/labs/jedd-wolchok ]
2=Peregrine Pharmaceuticals
ABSTRACT:
A viable strategy to treat advanced cancers includes transferring of tumor-specific T cells. T cells that recognize tumor antigens can be expanded and reinvigorated ex-vivo. Furthermore, autologous T cells can be genetically modified to express anti-tumor T cell receptors [TCRs] or chimeric antigen receptors [CARs]. Although the potency and specificity of tumor-specific T cells can be manipulated ex-vivo, once re-infused into patients, the T cells are subjected to immunosuppressive mechanisms established by the tumor. An important immune checkpoint regulator within tumors is phosphatidylserine (PS). Innate immune cells exposed to PS secrete suppressive cytokines and chemokines that can significantly impair the function and activation of anti-tumor T cells. Therefore, monoclonal antibodies that block PS activity can increase the anti-tumor potency of transferred T cells to treat aggressive cancers. Here we show that a PS targeting monoclonal antibody in combination with CD4+ T cells that recognize the melanoma antigen Trp1 can regress very advanced melanomas in all treated mice. Combination of anti-Trp1 CD4+ T cells with other immunomodulatory modalities such as anti-OX40 antibodies, can achieve equivalent treatment rates but these are typically accompanied by severe immune related adverse events. In contrast, in this setting, PS blockade did not show any off-target toxicities. Flow cytometry analysis revealed lower levels of CD206 expression concomitant with higher activation markers in macrophages and neutrophils in tumors from anti-PS treated mice. These results suggest that diminishing suppressive mechanisms locally in adoptive transfer protocols is a highly desirable strategy that can eliminate tumors while minimizing related adverse events.
---------------------
FROM PPHM’s 4-3-17 PR: http://ir.peregrineinc.com/releasedetail.cfm?ReleaseID=1019762
…”Latest Findings from Ongoing Collaboration with Memorial Sloan Kettering (MSK) Support Potential Applications for Combining CAR T & Anti-PS in Treatment of Solid Tumors”… For this study, a team of MSK researchers led by cancer immunotherapy thought-leaders, Taha Merghoub, Ph.D. and Jedd D. Wolchok, M.D., Ph.D., evaluated and compared the anti-tumor activity and off-target toxicities of adoptive T cell transfer therapy in combination with either PS-targeting antibodies or anti-OX40 antibodies in mice with advanced melanomas. Whereas PS-targeting and anti-OX40 demonstrated comparable tumor regression when administered in combination with transferred adoptive T cells, only the PS-targeting combination achieved these results without any off-target toxicities. By contrast, the anti-OX40 treatment combination triggered off-target inflammatory destruction of healthy tissues. Additional study results demonstrated that the PS-targeting antibodies decreased tumor-induced immunosuppression as evidenced by a decrease in immunosuppressive regulatory T cells (Tregs) and M2 macrophages. This finding is consistent with Peregrine’s belief that bavituximab may modulate the immunosuppressive tumor microenvironment and enhance the activity of immunotherapy agents.
Taha Merghoub, Ph.D., Co-Dir. of the Ludwig Collaborative Laboratory at MSK:
“While adoptive T cell transfer remains one of the most exciting new approaches to treating cancer, to date the toxicity associated with the treatment has limited its potential. We are encouraged that these study results showed that the combination of anti-PS and adoptive T cell treatment led to enhanced anti-tumor effect without any evidence of additional off-target side effects. “We believe that these findings may support potential applications for this combination in solid tumors in the future.”
Joseph Shan, Peregrine’s VP of Clinical & Regulatory Affairs:
“These study results provide further support for our belief that anti-PS agents such as bavituximab can play an important role as part of combination cancer treatments. This is directly tied to the agents’ ability to modulate the tumor microenvironment to combat the immunosuppression that limits the activity of CAR T and immunotherapies. Importantly, we are now also seeing evidence that this targeted modulation of the tumor microenvironment by anti-PS allows for enhanced activity of these other treatments without triggering any off-target toxicities. This is opposed to other conventional immunotherapies such as anti-OX40 with systemic mechanisms of action. We believe this advantageous tolerability profile will be a key benefit in positioning anti-PS agents for inclusion in optimal combination cancer regimens.”
---------------------
8-2015: Presently there are 3 types of Adoptive Cell Transfer (ACT) using effector T cells that are advancing on a path towards regulatory approval:
1. TILs (tumor infiltrating lymphocytes) have been developed with slow but continuing progress over several decades.
2. CARs (chimeric antibody receptors) – newer gene-modified T cells strategy
3. TCRs (T-cell receptors) – newer gene-modified T cells strategy
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4507286/

...“Adoptive T cell transfer is like ‘giving patients a living drug’,” states Renier J. Brentjens, MD/PhD, of Memorial Sloan Kettering Cancer Center (MSKCC).
… https://www.cancer.gov/about-cancer/treatment/research/car-t-cells
...“Adoptive T cell therapy (ACT) is one stone in this new pillar, a potentially powerful approach to cancer treatment that relies on the infusion of tumor-specific T cells.”
… https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4327320
= = = = = = = = =
Interesting 3-31-17 Sloan Kettering Tweet re: AACR’17
3-31-17 9:20amET “Getting ready for #AACR17? #Immunotherapy will be a hot topic. Learn more about how it works (video). @AACR”
https://twitter.com/sloan_kettering
Points to this 4-2016 Video (1:20):
“Immunotherapy – How It Works” https://www.youtube.com/watch?v=COQ1AeoGyco
Beg@:39:
“Immunotherapy drugs release this brake and empower immune cells to fight the cancer.
Sometimes the immune system needs a tune-up before it can fight cancer.
Immune cells can be removed from the body, armed with new proteins that can target cancer cells, and given back to a patient in large numbers.
Once inside the body, the modified immune cells recognize and attack the cancer.
This approach is called CAR T cell therapy. [an Adoptive Cell Transfer “ACT” strategy]
Despite the promise of immunotherapy, not everybody responds.
MSKCC scientists are exploring ways to improve immunotherapy.”

=============AND, THIS 3-23-17 PARKER FOUNDATION RELEASE ON AACR’17:
3-23-17: “Parker Institute for Cancer Immunotherapy Scientists to Present Research on Checkpoint Inhibitors, Adoptive Cell Therapy, and Other Advances in Immuno-oncology at AACR 2017”
Investigators affiliated with the Parker Institute for Cancer Immunotherapy will present some of the most anticipated immuno-oncology research at the 2017 AACR Annual Meeting. The event takes place at the Walter E. Washington Convention Center in Washington, DC, April 1-5 2017. . .
Other adoptive cell therapy abstracts of interest:
• ”Targeting Phosphatidylserine in Combination with Adoptive T Cell Transfer Eliminates Advanced Tumors without Off-Target Toxicities in a Melanoma Preclinical Model” [see http://tinyurl.com/nx5q5os ]
The principal investigator is Taha Merghoub, PhD, Parker Institute member researcher at Memorial Sloan Kettering Cancer Center. Co-authors include Parker Institute Center Director Jedd Wolchok, MD, PhD, at Memorial Sloan Kettering Cancer Center.
http://www.parkerici.org/media/2017/parker-institute-for-cancer-immunotherapy-scientists-to-present-research-on
----------ACT NOTES:
NOTE1:
From 3-2014 Immunotherapy article: “Cancer immunotherapy, particularly adoptive cell transfer (ACT), has shown great promise in the treatment of patients with late-stage disease, including those who are refractory to std. Therapies” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4372895
NOTE2:
The Parker Foundation: “The Immunotherapy Dream Team”
Through the support from SEAN PARKER, Stand Up To Cancer (SU2C) and the Cancer Research Institute (CRI) formed an Immunology Research Dream Team dedicated to cancer immunology: “Immunologic Checkpoint Blockade & Adoptive Cell Transfer in Cancer Therapy.” The Immunotherapy Dream Team is focused on 2 approaches for this translational cancer research project, which will unite laboratory & clinical efforts towards the immunological treatment, control, and prevention of cancer.
The 1st is investigating blockades (by inhibitory molecules called “checkpoints”) of T lymphocytes’ inhibitory receptors, which block immune responses; and the use of antibodies to remove the checkpoints, once again allowing white blood cells called T lymphocytes to kill the cancer cells.
Second, the Immunotherapy Dream Team is pursuing multiple Adoptive Cell Transfer (ACT) approaches, which increase immunity.”
DREAM TEAM LEADERSHIP: 10 scientists, incl. MSKCC’s Jedd D. Wolchok & Michel Sadelain.
http://parker.org/initiatives/immunotherapy









